Remicade is a common biologic that many IBD patients will try along their IBD journey. But starting a new medication can be nerve-wracking, especially if it’s the first time you’ve been on a biologic!
In this blog post, I share my experience receiving my first Remicade infusion. If you’re thinking about starting Remicade, keep reading so you know what to expect for your first infusion.
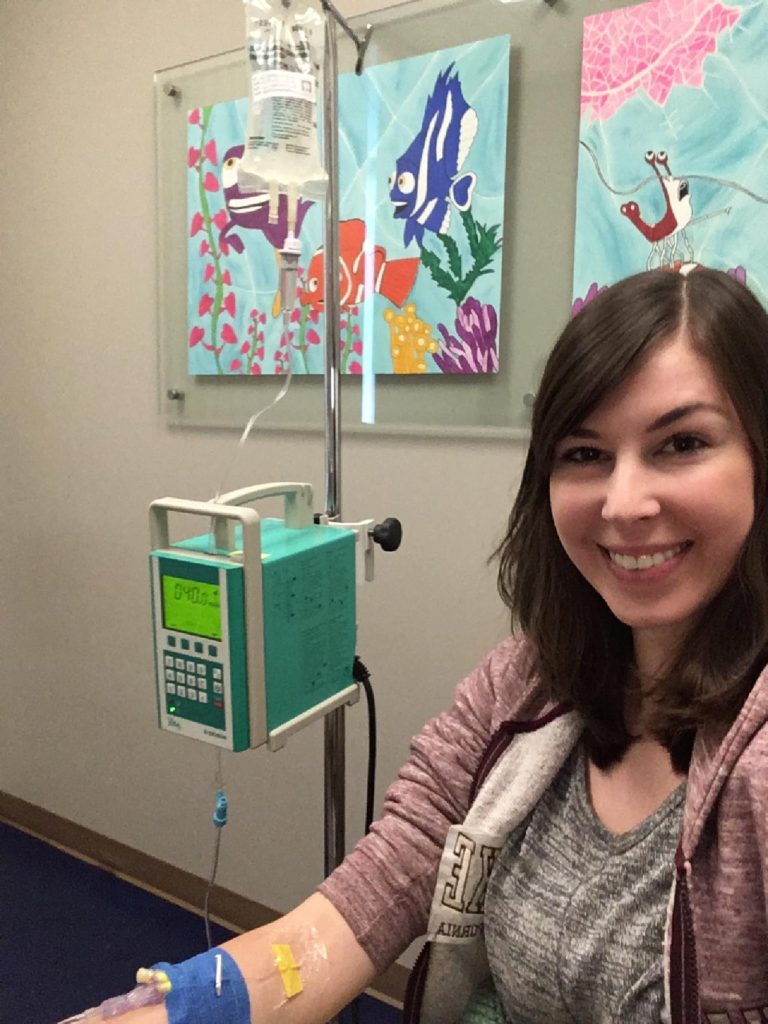
Feeling Nervous on My Drive to the Infusion Appointment
One fine day in March 2015, I missed class to go get my first Remicade infusion.
I drove myself to the hospital, hands clinging to the wheel. Nervous. Feeling totally unprepared. I had no expectations because I didn’t know what this experience would be like.
The drive felt like forever and five minutes at the same time. Finally finding a parking place after twisting my way through the intertwined roads of Sacramento, California, I drew in a breath. Pep talk time. Okay colon, I’m taking back the reins. If it takes sticking a needle into my arm and getting a medication placed directly into my veins, so be it.
Getting My Vitals Taken at the Hospital
I found my way to the waiting room and sat there nervously for a few minutes. Then I followed a nurse into the infusion ward. She took my temperature, height, and weight, explaining that they’ll take my weight before every single infusion because it determines how much Remicade you get that day.
I started with the lowest dosage, which is 5 mg per kg of body weight, which was about 280 mg for me.
The Infusion Ward Setting
Next, she led me back to the infusion room. There were a dozen chairs throughout the room with people hooked up to IVs.
I have to say, the mood was a bit dim. Remicade is typically dosed in the chemotherapy ward, so some patients were receiving cancer treatment and others were getting infusions for rheumatoid arthritis.
I sat comfortably in the cozy sofa chair and the nurse’s aid offered me a pillow and blanket. I said yes because it was freezing and I knew this would help relax me and take away some of my nerves.
Getting Blood Drawn
My GI sent orders for me to get blood drawn before every infusion. That way, my doctor can analyze these results to catch any abnormalities, deficiencies, inflammation, or signs that Remicade might not be working.
I also get my liver enzymes checked at every infusion, including CBC, CMB, CRP, GGT, and Sedimentation Rate.
It’s great to know my doctor always has eyes on what’s going on inside my body so we can catch things before they happen!
Taking 3 Pre-Medications to Prevent Reactions
Next, we started the process by taking my pre-medications: Tylenol, Benadryl, and Solu-Medrol. Solu-Medrol is basically an IV version of prednisone. (Don’t worry, it’s not enough to give you moon face or the other awful prednisone side effects).
The purpose of these three medications is to reduce the chances of getting negative side effects from the Remicade.
Specifically, they help prevent the patient from experiencing hypersensitivity, which is the immune system’s exaggerated response reacting to a foreign agent (Remicade) entering the body.
The chances of hypersensitivity are even higher during your first infusion, so I really needed to get these meds into my system. I took the Tylenol orally, but the Benedryl and Solu-Medrol were given through my IV.
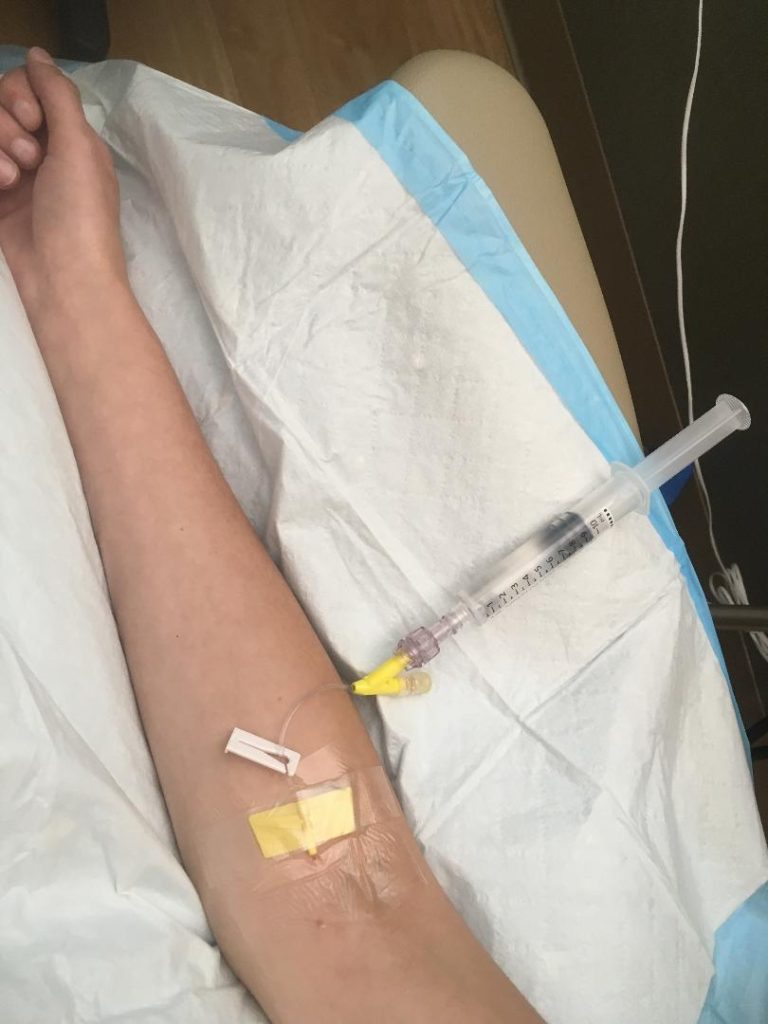
Feeling Drowsy from the Benadryl
If you’ve taken oral Benedryl, you know how quickly it can take effect. Now imagine it pumping straight into your bloodstream!
I immediately became extremely sleepy. My eyes closed, my head nodded, and speaking became a chore. The nurse squeezed it slowly through the syringe and I felt peaceful and relaxed for the first time in what felt like forever.
Starting the Remicade Infusion
Once these pre-meds were absorbed, they switched out the syringe for a long IV tube attached to a monitor on wheels. The nurse taped the tube to my shoulder and on my forearm so that it was easier to manage and less likely to tangle.
The Infusion Was Surprisingly Relaxing
I remember the nurse explaining that now the Remicade will be entering through the IV; my sleepy ears heard her and I nodded with my eyebrows raised high but my eyes unable to open.
The bag of Remicade hung from the top, and—still drowsy—I remember seeing the clear liquid drip, drip, drip, down the bag, through the plastic tube, and straight into my veins.
It felt kinda surreal. In this peaceful dream-like state, I paradoxically felt both relaxed and anxious. Relaxed from the Benadryl, but anxious that I was attached to this machine for three hours.
I pressed into the peace, focusing on this time that I could just be.
No homework. No studying. No organizing my next week’s medications into my pillbox.
It was a peace I had become unfamiliar with. Like a part of me that my disease stripped away was being reconnected. I let my thoughts wander as I fell into a wonderful sleep.
Periodically, the machine would beep, and the nurse would stop by my station to turn the alarm off. She’d check on the infusion’s progress, increase the rate, and take my blood pressure. Then back to sleep I’d go.
This is how it went for the three hours.
Lunch Time at the Infusion Ward
The final time I awoke, the nurse’s aid was standing by me, offering food! Hospital food is not known for its quality, but for some reason, this sandwich was so delicious!
This simple chicken sandwich, this plain-Jane bread with a single tomato slice and a sole lettuce piece, was absolutely amazing. For whatever reason—the pre-meds, the Remicade itself, or perhaps the long nap—made this sandwich oh so fulfilling. The food woke me up and by then, the Benedryl had worn off.
“All done!” the nurse chimed.
She extracted the needle from my skin and removed the blue tape that had secured the long IV to my arm.
OUCH! I have no doubt that yank took some arm hairs with it. To be honest, that tape removal was so much more painful than the needle’s poke!
How I Felt Immediately After the Infusion
After the nurse placed a Band-Aid over my war wound, I gathered my things and walked out of the hospital awake, (energized actually!) with my veins flowing with sweet, sweet Remicade.
I have to say, I felt better immediately. Even during the infusion. I felt like it was putting my body back together. Like my colon was a broken puzzle and Remicade was the mastermind who could make it whole again.
What I’m trying to say is that I hadn’t felt this good in a long time.
How I Felt Over the Next Two Weeks
This goodness continued throughout the next two weeks before my second loading dose infusion.
I was able to make plans AND stick to them.
I was able to enjoy my time away from my apartment.
I was no longer scared of being without a bathroom during 10-minute car rides.
I had normal bowel movements! Like from the good ol’ days of pre-diagnosis. I told my parents that I will never take a normal poop for granted again. It’s the little things in life, guys 🙂
And Remicade—the scary IV drug I initially dreaded—reminded me of this. It boosted my quality of life and gave me the freedom that I had forgotten I once had. From day one, it began to stitch hope back into my life.
Questions about My Remicade Experience?
I hope you found this blog post helpful! Do you have questions about something I didn’t cover here? Drop a message in the comment section below, or reach out to me privately here. Chat soon!
Related Posts
Great post! It made me cry. I’m getting my first Remicade infusion this Thursday. I have had UC for 12 years and always dreaded the day I might have to go on a biologic, but now I’m (mostly) ready for it. I really want to get off prednisone!
Thank you for your kind words! You’re not alone, I had that same reaction when I was first told I needed to start biologics; it’s such a different territory. But the nurses will make you comfortable, especially if you tell them it’s your first time 🙂 (My advice is to always ask the nurse for a blanket, pillow, and hand warmer, if they have them available. It can be chilly in there and those things always help me relax, too). I’m sure your infusion tomorrow will go smoothly, and I hope Remicade is your forever drug 🙂 I’ll be thinking of ya!
Thanks for the super nice and supportive response! It went fairly well yesterday. I felt a bit lightheaded at the end of the infusion and for about 2-3 hours afterwards but not too terrible. My blood pressure dropped to 88/53 by the end of the infusion, but the nurses didn’t seem worried at all. I was worried so I called them and they told me I could come back in and have them re-check my blood pressure 1.5 hours after the infusion and it was up to 104/63, so closer to normal for me. I have a lot of anxiety about the possible side effects of this medication. 🙁 They didn’t keep me afterwards to monitor me or give me pre-meds, and I didn’t get a super comfy recliner chair or any privacy. I was in a room with other patients getting IV infusions. So that was a bit of a bummer but oh well.
This surely made me feel better, I’m having remicade infusions because I have severe rheumatoid arthritis disease that has many caused problems and surgeries.
I hope your infusions bring you relief, Tamara!
My daughter received her first infusion eight days again. Initially felt amazing but that only lasted a few days. Now back to being sick… she has to get a stronger dose this time in 5 days and we’ll see how it goes. I’m praying it helps her she’s only 16 and has only had UC for 6 mos and no meds have worked thus far. Humira is the next option but I’m hoping to God that hit his stronger dose of Inflectra will do the job! Thanks for your amazing story it’s given me hope. ??
Hi Nina. Thanks for sharing this! Starting a new biologic can be really stressful. When I first started Remicade, I also felt a difference right away, but it took a couple doses to bring me into remission. I hope that Remicade starts working for your daughter very soon ? And it’s great that her GI already has a backup plan in place just in case. Will be thinking of you two!
My boyfriend is receiving his first infusion soon after several years on Humira. I didn’t even know there were long term non-biologic medications for UC, because after they reduced the inflammation with prednisone, he immediately went on Humira, and that’s the only thing that’s been keeping him upright for the past 3 years. It’s just getting too tedious and expensive. I’m glad to have found this article. It’s comforting to me, and therefore I can be a comfort to him through this experience. I was terrified of the state he was in prediagnosis and the diagnosis felt like a death sentence (though he’s more or less a success story to his GP and GI, fingers crossed that continues), but knowing there are people getting on (at least relatively) fine is nice to see, people who make light of some experiences bystanders might find see much differently. I know he sees this all differently than I do, as he sees my problems differently than I do. It’s just nice to get some perspective. Thank you for being honest and open.
Hey Agnes, thanks so much for your kind words! I’m so glad to hear this article was helpful. I’ll be thinking of you guys as your boyfriend starts his biologic. I’ve been on two biologics so I know the transition from one to the other isn’t fun, but in the end I hope the new medication brings him relief! If you two ever have questions, don’t hesitate to reach back out! Stay safe and be well ?
I am getting my first Remicade infusion for Crohn’s tomorrow and this really helped ease my anxiety about it! Thank you so much for writing this! You’re helping a lot of people by sharing your experiences and insight.
Hey Claire! I’m so happy that you found this helpful! I hope your infusion today goes smoothly and brings relief! You got this! ?
This blog is such such an amazing resource for me! I am getting my first infusion tomorrow for my Crohn’s. I am a bit nervous, but more excited! I can’t wait to be on the journey to remission. I was only diagnosed a month ago and things are moving so fast. This was so helpful to let me know what’s gonna happen tomorrow!
Hey there! Thanks so much for your kind words, I’m so glad you found this blog post helpful 🙂 I hope your infusion went smoothly yesterday and that Remission brings you relief very quickly. I’m always here if you have questions, and welcome to the IBD community ?
This was very helpful. My 18 year old daughter is starting her first dose of Remicade tomorrow. She was just diagnosed with Crohn’s in April when she was hospitalized with a stricture. Hers is in her terminal ileum. It is good to know what to expect. Thank you.
Thanks for your kind words, Renee! I’m so happy to hear this post was helpful. I hope your daughter’s infusion went well yesterday and that Remicade brings her relief ?
I had my first infusion today and felt everything that you described in this post. I was looking for how people that had infusions slept the first night. No aches and pains since having the infusion this afternoon. Feels like a miracle!
Hi Debbie, it’s good to hear from you! Thank you for your kind words and I’m glad to hear you’re feeling great after your infusion! I hope it continues to bring you relief for a very long time!
This is soothing. I have Stage 3 Hidradenitis Suppurativa, and currently on Humira. My first Remicade infusion is next Friday. NYC based I am. Luckily I have the next 10 days come next Friday to myself.
Thanks for your kind words! Sending you warm wishes and I hope your first Remicade infusion goes smoothly!
Thank you so much for sharing your story. I am in the beginning stages of determining if I want to move forward with infusion therapy for ulcerative colitis. I am tired of dealing with the issues I’ve been dealing with the last 3 years, especially being held hostage by my bathroom. I appreciate your transparency and honesty through your testimony. I’m ready to start feeling better and back to the “old” me.
Thanks for your kind words, Melissa! I’m thinking of you as you start your infusion medication. I really hope whichever biologic you decide to go with brings you relief! I know how disheartening it can be to be tied to the bathroom. Here’s to getting back to the old you!
Thank you so much for you article, it has really made a old man (77) feel a lot better. I am Scheduled for first infusion on the 18th. June this year and been having lots of anxiety about it. My Humaria quit working so this is what Doc. recomended. Have had this uc for twenty plus years, so hope this works out. Thanks for your knowledge about Remicade.
You’re so welcome, Dale! I’m really glad to hear it. I hope your first Remicade infusion went smoothly and that it brings you relief!
Thanks for the post. Today was my first infusion and I was fearful at first. Your blog helped. I was told I should not drive home and although they didn’t check like when you get a Colonoscopy, I was glad I didn’t drive. I will also tell my Doc to do the Liver enzymes blood work next time!
Thank you Brian! I’m so glad you found this post helpful and I hope your first infusion went smoothly! They’ll start to feel like second nature over time.